An ectopic pregnancy occurs when a fertilised egg implants itself in other organs, that is not in the uterus where it is supposed to. Most commonly the egg implants itself in the fallopian tube. This is the tube that connects the ovaries with the uterus. The tube is narrow, and the environment is not suitable for the embryo to grow as such most ectopic pregnancies are not viable and have to removed surgically or through medication. If a woman has been diagnosed with an ectopic pregnancy but is healthy with no worrying symptoms, then the doctor can discuss the options available with different Ectopic pregnancy treatments.
The blood pressure and pulse need to be within the normal limits without pain, bleeding or dizziness. But unfortunately, an ectopic pregnancy isn’t usually caught without the usual symptoms. So, if the woman is in severe pain, bleeding heavily or is fainting, then the doctor suggests an exploratory surgical option called laparoscopy or keyhole surgery. This allows him to see what is happening inside the woman’s body.
New treatment methods have been developed to deal with this issue, and there are a few options to try.
Risk Factors
There are risk factors that are strongly associated with an ectopic pregnancy. These include tubal surgery, exposure to in utero diethylstilbestrol or a previous ectopic pregnancy. Current smoking habit and a history of infertility or genital infections are also a huge risk. Contraceptives can reduce the risks for ectopic or intrauterine pregnancy. Still, previous use of an intrauterine can cause an ectopic pregnancy as it doesn’t allow the fertilised egg to implant in the uterus.
Ectopic Pregnancy Treatments
An ectopic pregnancy is a high-risk condition that currently occurs in 1.9% women, those who report it. It is a condition when a pregnancy occurs outside the uterine cavity. For more detailed information, read our blog everything you need to know about Ectopic Pregnancy. It is one of the leading causes of pregnancy-related deaths in women during the first trimester. Usually, a woman in reproductive age who faces vaginal bleeding, abdominal pain, hypotension or syncope, may have it, and the doctor must conduct a pregnancy test.
If the patient does happen to be pregnant, then he has to test for ruptured or possible ectopic pregnancy. An ultrasound evaluation, along with human chorionic gonadotropin levels, can also help in the confirmation of diagnosis. The following are the ways or methods through which an ectopic pregnancy may be managed.
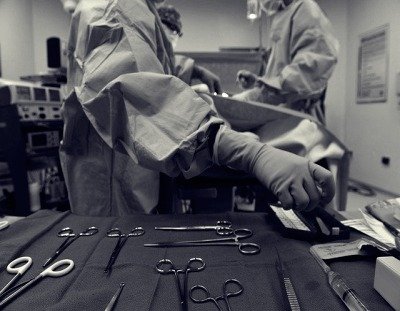
A – Surgical Management
This is a very established form of treatment for an ectopic pregnancy. It means performing a surgical procedure or operation to remove the ectopic pregnancy while the patient is under general anaesthesia. If beta hCG or the pregnancy hormone level is high, there is significant internal bleeding or the ectopic is large then the doctors cannot consider a less invasive treatment as the patient’s health may be at risk and surgery is the only available option. A surgical procedure is also the third option is medication, and expectant management has failed.
-
Laparotomy
Surgery traditionally involves a Laparotomy or an open cut on the lower part of the abdomen, very similar to a c-section. This may still be used in case of rupture or heavy bleeding or if there is a lot of scar tissue, then this procedure may be performed in emergencies. A blood transfusion may be given if there is excessive bleeding.
-
Keyhole Surgery
But in most circumstances, a procedure known as laparoscopy or keyhole surgery is performed. A camera is inserted through the belly button and instruments are inserted through cuts in the lower abdomen. Some gas may also be added to inflate the abdominal cavity so that the surgeon can see the inside of the abdomen.
- Salpingectomy
Once the surgeon has seen the damage inside the abdominal cavity and chooses an option depending on the condition of the affected tube and the other tube. If the second (unaffected) tube is fine, then the tube affected by the ectopic pregnancy is removed. But if the second tube is also not alright, then the only option is to remove the ectopic pregnancy from the tube by using a small cut, but leaving the tube as is. This procedure is known as salpingotomy.
It may not always be viable to perform a salpingotomy as there is a small risk that some of the ectopic tissue remains and the patient may be advised blood tests to monitor the hCG levels as they are decreasing, and pregnancy issue is resolved. If HCG levels are not decreasing, then further surgery or a drug prescription may be required.
The patient may be required to stay in the hospital for one or two days after laparoscopy or keyhole surgery and for 2-3 days in case of laparotomy or a cut to lower tummy. After discharge, the medical practitioners will advise on diet, exercise and aftercare. The stitches usually dissolve within a week.
B – Medical management with Methotrexate
Usually, medical management is used as a term when the drug methotrexate is used. An essential vitamin called folate is required for the rapidly dividing cells that occur during pregnancy. Methotrexate interferes with the processing of this vitamin. This drug can prevent the pregnancy from progressing, and the body will gradually absorb it, leaving the fallopian tube intact.
The drug is most effective in the early stages of pregnancy, usually when the beta hCG is below 5000 mIU/mL. If the levels are higher than this, then there is a risk of rupture. In the case of corneal ectopic pregnancy, it is common to treat the pregnancy with this drug even with higher hCG levels. In an ectopic pregnancy, the size of the growth is more important than the gestation period.
The drug is given through injection, and the dosage depends on the woman’s height and weight. A test to check for anaemia is also performed before the administration of Methotrexate. The method is used to avoid surgery, but it requires monitoring as well as follow-ups. The patient has to visit the hospital, and the hCG levels are monitored for several weeks until they are negative.
The hCG levels are usually tested on the day the drug is administered and then again on day four, followed by day seven. The hCG levels may arise on the day as the cells have still been dividing, and some cells may release more hCG as they begin to disappear. The doctors expect a drop of 15% in hCG levels between day four and day seven. If this level of reduction is not seen, then a second dose of the drug may be administered.
Women may also bleed for a few days after the injection, and it can last for six weeks. The hCG levels are monitored every 3-7 days, and most women need only one injection. This procedure is as good as surgery for future pregnancies as it is non-invasive.
C – Expectant Management
Expectant management is close monitoring or watchful waiting instead of immediate treatment. For patients that are assessed properly and whose beta hCG levels are dropping, then at least half of these pregnancies end naturally. To decide if this method is best for a patient, the doctors would look at blood tests, general health and ultrasound scans. Expectant management is considered only under the following circumstances:
- stability in general health
- the beta hCG levels are low
- the ultrasound shows a small ectopic pregnancy with no significant bleeding
- pain levels are normal
Doctors keep testing the blood to ensure that hCG levels are dropping and it can take from 2 weeks to 3 months for hCG to fall back to non-pregnant levels. Most women get back to a non-pregnant state in the 4th week.
FAQs
-
How does the patient feel after surgery?
Women can experience some pain 1 or 2 weeks after the surgery and this manageable with painkillers. If the woman has had a laparoscopy, then she may feel bloated for a week and experience pain that is similar to trapped wind. This happens because of the gas that is used during the surgical procedure. The patients may feel tired due to blood loss, and if they are given iron tablets, then the stools passed will be black, and the patient may also feel constipated.
-
What can be done to recover from surgery?
For the first few days after surgery, the patient has to move gently, but walk around a little daily, gradually increasing the distances you walk. The nurse will advise on caring for the wound area like if they are dissolvable or you need to return to have the stitches removed. Women can take a shower after 8 hours post-surgery and need to keep the wound area clean. Until the wound has healed, the patient must not do any heavy lifting or vigorous housework or even exercise vigorously.
The hospital may also advise on using Kegel or pelvic floor exercises to recover a normal bladder tone. Most take time off from work for at least two weeks to heal and deal with this emotionally.
-
How do doctors monitor the patient after surgery?
If the patient has had one fallopian tube left or if there is any doubt in whether all the remaining tissue was removed, then the doctor may monitor the hCG to make sure that they are going down. High hCG levels may mean that the pregnancy or tissue remains. This test is done a week later. If the fallopian tubes have been removed, then no monitoring is needed, but the hospital may still call the patient back to check on the wound, six weeks after surgery. The GP may see the patient before they resume work to check on the healing.
-
What are the risks and side effects of Methotrexate?
The risk for this method is that the medicine may not actually work, and the cells may continue to divide, which would mean that there could be a need for surgery. The known success rate is around 65%-95%. They tend to be higher when the serum hCG levels are lower. Occasionally an ectopic pregnancy may rupture despite low hCG levels.
There are a few common side effects of Methotrexate, such as:
- fatigue
- cramping or severe abdominal pain that occurs during the first 2 to 3 days of treatment
- indigestion, vomiting and nausea
- spotting or vaginal bleeding
- sore bottom or numbness from the injection
- dizziness or lightheadedness
- inflammation of the membrane covering the eye
- temporary hair loss or sore throat and mouth
- skin sensitivity to natural light
- lung inflammation
- severely low blood count
-
Is medication suitable for me?
This treatment is suitable if the woman is:
- in good health
- the tube hasn’t ruptured
- no severe abdominal bleeding
- low hCG levels
This method is better over surgery in case of the following reasons:
- there are adhesions in the pelvis or abdomen
- other medical issues that increase the risk in general anaesthesia
- the location of the ectopic pregnancy is in the neck of the womb or as the tube that enters the womb
Methotrexate is not suggested if the patient has any of the following conditions:
- shortage of blood cells or severe anaemia
- kidney or liver problems
- ongoing or active infection
- ulcerative colitis or peptic ulcer
- AIDS/HIV
For the treatment to work, the patient must stop consuming minerals, vitamins or other medicines unless advised by the doctor. It is particularly important not to take any folic acid supplements. Do not perform any strenuous activities unless the hCG levels have dropped and avoid any sexual activity until you are at the non-pregnant stage. Avoid painkillers such as ibuprofen and alcohol is also not allowed.
-
What are the risks of expectant management?
The main risk under this procedure is that the cells will continue to divide, which means that there could be a need for surgery after the period of expectant management. Data shows that 25% still need surgery or drugs after the initial expectant management. Sometimes an ectopic pregnancy can rupture despite low hCG levels, and you must contact emergency services at that time.
-
How to know if expectant management is not working for me?
Regular blood test tells doctors if your pregnancy is progressing or being resolved. A deteriorating ectopic pregnancy means there will be shortness of breath, pain, and bleeding. If you feel any of these symptoms, then you need to be reassessed.
-
How to make expectant management work for me?
When hCG levels are dropping, then the woman mustn’t take up strenuous activities. Until the doctor is confident that the pregnancy is resolving, do not undertake sexual intercourse. Don’t take folic acids or supplements or any other minerals.
Reference Links
- Surgical Treatments of Ectopic pregnancy: Reference from ectopic.org
- Risk factors related to Ectopic pregnancy: Reference from aafp.org




Leave A Comment